Policy bite - universal health coverage
 español
español
Professor Amanda Howe, our new President–Elect, said in her speech at the WONCA Council that she would “help with policy messages. In WONCA …. we know what we want to say. I’d work on how we say it – getting accurate clear briefing documents out, so you can adapt them for use in your place”. So now we are inviting her to take up that challenge. Here is Amanda’s second offering, and she will do this regularly.
We are also inviting you to send us similar material - an important piece of policy from your own organisation or setting that relates to family medicine developments and that might be helpful to others. Please send a summary, a link, and make it short - its not Twitter, we shall allow up to 500 words! Each piece will be reviewed to check it is appropriate to publish it on the public part of the website - you can also log in to the members' forum to discuss reactions and related issues.
Universal Health Coverage
In December 2012, following the publication of the 2010 World Health Report by the World Health Organization (WHO) on 'Health Systems Financing: The Path to Universal Coverage', a UN resolution was passed encouraging governments to move towards providing universal access to affordable and quality health care services. Most recently the 2013 World Health Report has been published on the subject of 'Research for Universal Health Coverage'.
What does Universal Health Coverage mean?
In essence Universal health coverage (UHC) aims to ensure everyone has access to needed promotive, preventive, curative, palliative and rehabilitative health services of sufficient quality to be effective without suffering financial hardship as a result. The WHO outlines that:
“For a community or country to achieve universal health coverage, several factors must be in place, including:
- A strong, efficient, well-run health system that meets priority health needs through people-centred integrated care (including services for HIV, tuberculosis, malaria, non-communicable diseases, maternal and child health) by:
- informing and encouraging people to stay healthy and prevent illness;
- detecting health conditions early;
- having the capacity to treat disease; and
- helping patients with rehabilitation.
- Affordability – a system for financing health services so people do not suffer financial hardship when using them. This can be achieved in a variety of ways.
- Access to essential medicines and technologies to diagnose and treat medical problems.
- A sufficient capacity of well-trained, motivated health workers to provide the services to meet patients’ needs based on the best available evidence.
It also requires recognition of the critical role played by all sectors in assuring human health, including transport, education and urban planning.”
In order to do this funds need to be collected and pooled (e.g. through taxation or social health insurance), and then used to pay for services, such as primary care, that meet the requirements outlined above. In the provision of health services three key dimensions need to be considered:
(1) Who is covered?
(2) Which services are offered?
(3) What proportion of the costs are covered? (see Fig 1),
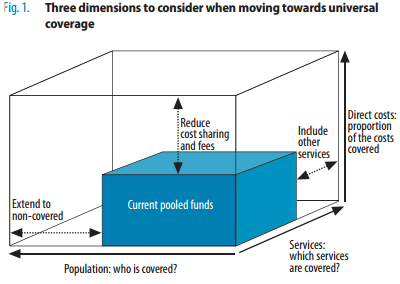
Source: The world health report 2010. Health systems financing: the path to universal coverage. Geneva, World Health Organization, 2010.
The 2013 World Health Report addresses important questions about prevention and treatment, how services can be paid for, their impact on the health of populations and individuals, and how to improve health through interventions both within and beyond the health sector. It uses case studies from around the world to illustrate this and highlights the importance of communicating the evidence-base to change agents, authorities, opinion leaders and innovation champions, all of whom play different roles in policy-making and front line implementation.
Why is this relevant to family doctors?
WHO states that "a strong primary care system is central to an effective health system", so we need to be able to communicate the evidence on the value of primary care and use this to support and further develop primary care in all health systems in order to equitably and efficiently achieve UHC. Also, research needs to take place in communities in primary care settings - this is something that WONCA's Working Party on Research is already supporting, and WONCA welcomes case studies from your situation that will illustrate the successes and barriers in strengthening primary care and family medicine.
Your views?
Send your case study to Prof Amanda Howe, President-Elect [email protected]
Or to give your views login or join the WONCA forum
Login to the WONCA forum
Join the forum